Posted February 06th 2024
It is estimated that around 70% of the 1.2 billion women over the age of 45 in the world develop neurological and psychiatric symptoms during the perimenopause (the years before the final menstrual period).
The perimenopause is marked by unpredictable fluctuations in reproductive hormones, and cycles without ovulation which can typically be expected to last for around five years.

Research also suggests that perimenopausal women are at a higher risk of developing major depression, schizophrenia, or bipolar disorder, whilst women who already have a diagnosis will experience a worsening of symptoms.
However, there is little and often inconsistent information available on the link between the perimenopause and mental health, and what might predispose someone to become unwell during this transition to the menopause. This lack of information poses a major risk to women, their families, and health professionals.
For the first instalment of this series, we were joined by Professor Arianna Di Florio, Lisa Shitomi-Jones, Dr Clare Dolman to discuss how the menopause can impact mental health through research and a lived experience perspective.
Watch the full webinar online now
The perimenopause – lots of interest but little evidence
The association between the menopause and mental illness is described by Professor Arianna Di Florio as often trivialised and misunderstood.
“We know that over 50% of people going through the menopause experience neuropsychiatric conditions, such as depression and insomnia.
However, the mechanisms behind experiences of mental ill-health are different from person to person, which makes providing a broad treatment for all difficult.
Providing honest answers also becomes increasingly difficult when looking at the existing scope of research on menopause and mental illness, as the majority of which are reviews or case studies of previously collected data.
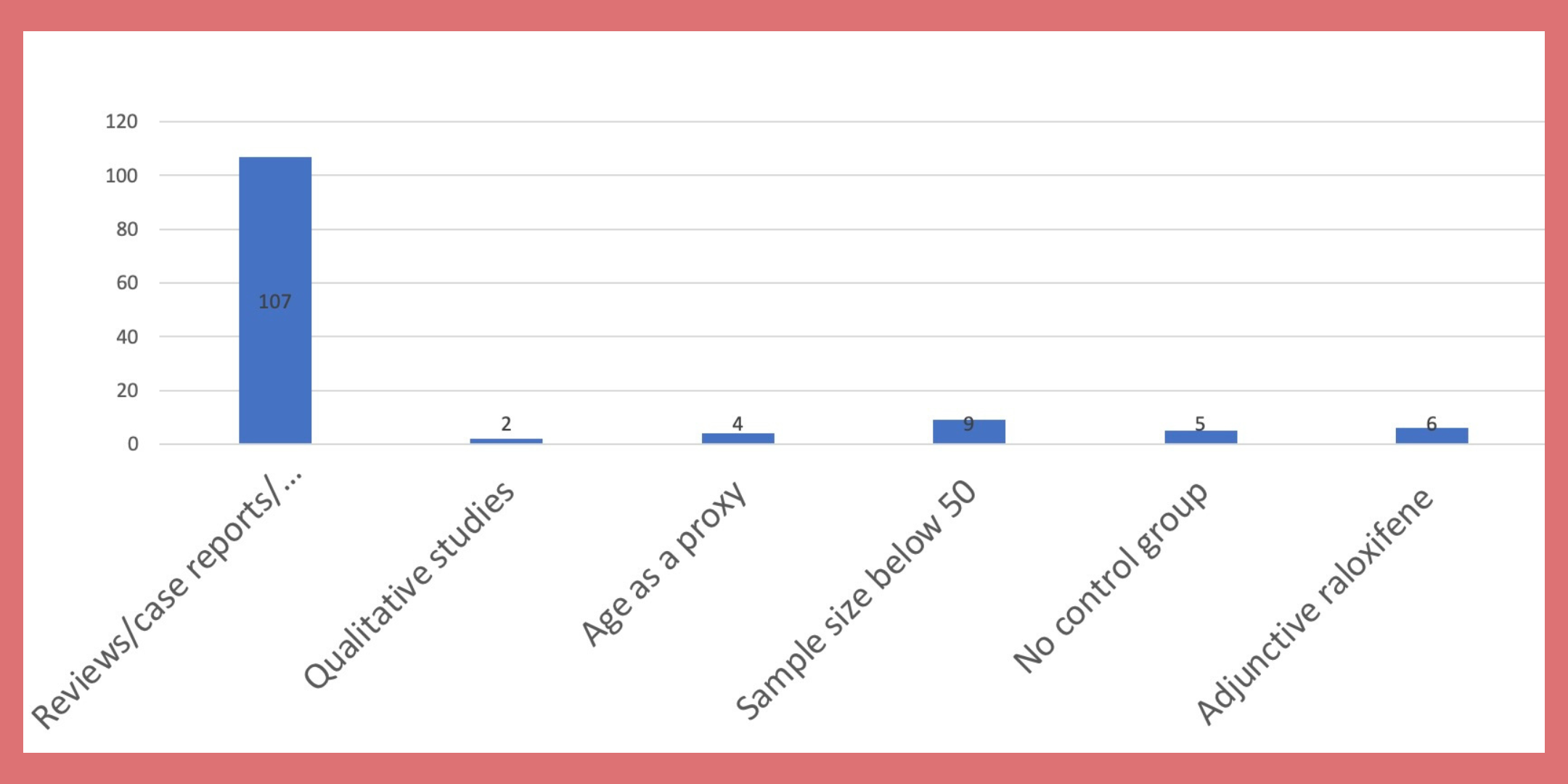
This led researchers working on the Reproductive Mental Health Programme at Cardiff University, Professor Arianna Di Florio and Lisa Shitomi-Jones, to further investigate the risk of developing a mental illness during the perimenopause.
“The key question behind our research is to ask if the perimenopause is really a period increased risk of mental illness.”
Is there a direct link between the perimenopause and mental illness?
So far, the research conducted at Cardiff University has looked at links between the perimenopause and specific mental health conditions like major depressive disorder, anxiety disorders, mania, and schizophrenia, as opposed to symptoms more generally associated with depression.
Pooling together information from an existing dataset, UK Biobank, the initial research has identified a heightened rate of mania (bipolar disorder) during the perimenopausal period.
However, what is interesting is that those who are at a heightened risk have no previous experiences of mental ill-health.
So, what does this association between bipolar and the perimenopause mean?
Professor Di Florio is curious to further investigate if this heightened risk of bipolar can be directly associated with the perimenopause, of if this is due to the ageing process at this life stage more generally.
“Although the most common psychiatric presentations around the perimenopause are related to depression and anxiety and bipolar disorder is on the rare side, the link is still quite specific.
“The consequences of developing bipolar disorder in middle age can be devastating, because most people don’t think it can be possible at this stage in life,” Professor Di Florio continued.
So far, Professor Di Florio has used this background of research to open a UK-wide second opinion women’s mental health clinic, based in Cardiff.
This free of charge service provides consultations for women experiencing mental illness that is associated with reproductive life events like menstruation, childbirth, and menopause to allow them further support in diagnosis and treatment.
Find out more about the Cardiff University Psychiatry Service (CUPS)
Menopause education is needed at a national scale
Dr Clare Dolman, a researcher based at King’s College London with lived experience of bipolar, discussed how the current views on the menopause in society:
“It’s only recently that public awareness has been raised about how debilitating and life-changing the menopause can be for many women.”
However, this awareness is very much needed due to the plummeting numbers of professional women leaving the workplace during the menopause because of the severity of their symptoms.
“Almost 900,000 women have left their jobs because of menopausal symptoms.”
If enough was known about the impact of hormones on the brain, it could be possible to predict which women would be more likely to develop severe symptoms in times of hormonal flux, like childbirth or the perimenopause.

This is the critical information that doctors and clinicians, as well as patients, need to know in order to be proactive before reaching the perimenopause and potentially becoming unwell.
To address the lack of knowledge and research surrounding the menopause and mental health, Bipolar UK recently launched a national commission which included a section of research dedicated to women of menopausal age.
This data revealed that 89% of women asked said they had never been told by a heath professional they were more likely to have an episode of bipolar at this time.
The full commission is available to read via Bipolar UK.
Learn more and watch the full webinar online now.
Don’t miss out!
The next instalment in the Women’s Winter Webinar series will be discussing the latest on how hormones can impact mental health, including the latest in premenstural dypsphoric disorder (PMDD) research.
Reserve your space via Eventbrite.
Read more
- Padlet | Resources and links mentioned in the webinar
- Cardiff University | Reproductive Mental Health Programme
- Bipolar UK | Learn more
Sign up now and receive new blog posts to your inbox.
